Common Presentations in the Head and Neck
Lumps in the head and neck FAQ
written by Dr James Kong
(Last update on: Oct 28th 2020)
Lumps in the head and neck are common and the cause is usually benign. Nevertheless these may be the presentation of either a malignancy or a chronic infection. If these abnormal structures persist for more than two weeks and there is doubt as to the cause, then the patient should be referred for specialist assessment. Patients over the age of 40 are more likely to have a neoplastic cause. Inflammatory, congenital and traumatic causes are more common in younger patients but neoplasm should still be considered. [1] If a cancer is present, early detection provides the highest chance of successful treatment.
Introduction
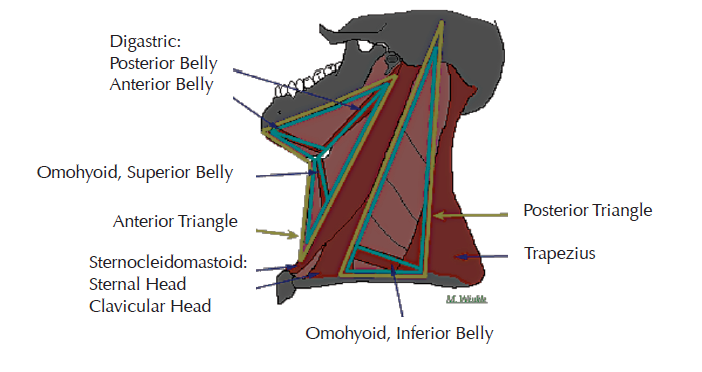
Anatomically, the sternocleidomastoid muscle divides the neck into the anterior and posterior triangle. The thyroid gland and its related problems will be one of the more common causes of an abnormality within the anterior triangle. These are usually asymptomatic and is often discovered incidentally by the patient. Lymph nodes are usually discovered in the posterior triangle of the neck and are not always serious. They are generally painless, despite enlarging steadily. The causes are usually infection or inflammation. Cancers that begin in the head or neck usually spread to lymph nodes in the neck before they spread elsewhere. For this reason, a lump in the neck that lasts more than two weeks, needs a comprehensive investigation.
 |
What Causes Head and Neck Masses?
There are numerous causes of head and neck masses.
Lymph nodes - this is the most common cause of new neck masses. Lymph nodes can enlarge when there is an infection and when this recedes, the (reactive) lymphadenopathy will subside but does not usually reach the original size.
Benign masses - although they do not metastasize, can still be serious if they impact on nerves or exert pressure in the head and neck, and may often need to be removed surgically. These include cysts, thyroid masses, vascular masses, salivary gland and others.
Cancers - head and neck masses are malignant, or cancerous, if they spread to surrounding tissue. These tumors may be either primary or secondary that originate in the head or neck itself, including the thyroid, pharynx, larynx, salivary glands, brain, and/or other locations.
Primary tumors of the head and neck typically spread to the lymph nodes in the neck. About 90% of head and neck cancers are caused by tobacco and alcohol use, and the deaths from these cancers are largely preventable. Cancers of the mouth and throat are nearly nonexistent in adults who do not smoke or drink. People who have been exposed to radiation, either during medical treatments as children (common in decades past) or from nuclear radiation sources, are at considerable risk for thyroid cancer and should be screened regularly.
Secondary cancers are tumors that have spread from primary tumors in other parts of the body to the head or neck. Most often, secondary tumors of the neck originate in the lung, breast, kidney, or from melanomas in the skin. Cancers in the nasal and sinus passages may spread to the brain through nerves in the skull.
Salivary glands - form the next largest group which present with a swelling. The most common salivary gland affected is the parotid and the vast majority (>90%) are benign and the majority of these are pleomorphic adenomas. A face-lift approach for parotidectomy which minimize the visual surgical scar is the preferred approach today. [2]
Symptoms Associated with Neck Lumps
- Lump in the neck persisting for more than two weeks, especially if it is not associated with a cold, flu, or other infection. Cancers of the mouth, throat, voice box (larynx), thyroid, and some lymphomas (blood cancers) can appear first as a painless, growing neck lump.
- Change in voice including hoarseness that persists more than two weeks
- Growth in the mouth
- Swollen tongue
- Blood in the saliva or phlegm
- Swallowing problems
- Changes in the skin – a dermatologist examining changes in the skin that could indicate basal cell carcinoma, squamous cell cancer, and malignant melanoma. Skin cancers are associated with prolonged exposure to the sun; most squamous cell cancers occur on the lower lip or ear.
- Persistent Ear Pain or ear pain while swallowing -- may be a symptom of infection or a growth in the throat
Diagnosing Head and Neck Masses
Although often no treatment is required… appropriate investigations should be undertaken to ensure that where necessary treatment is not delayed. [3]
Ultrasound and US Guided biopsy – is the investigation of choice. Serial ultrasound scans is a useful monitoring tool.
Neurological exam – includes evaluation of eye movements, hearing, sensation, muscular movement, sense of smell, balance and coordination.
MRI – Magnetic Resonance Imaging can clearly show tumors near bones, smaller tumors, and brainstems masses.
CT Scan – Computed tomography although less accurate than MRI, can help locate tumors or determine their types, detect swelling or bleeding, and evaluate the effects of treatments. Injections of iodine contrast material may be used to enhance the visibility of abnormal tissue during CT scans.
PET (Positron Emission Tomography) and SPECT (Single Photon Emission Tomography) – are useful after diagnosis to help determine the grade of a tumor or to distinguish between cancerous and dead or scar tissue. They involve injection with a radioactive tracer.
Treating Head and Neck Masses
Treatments are determined by the cause of the mass. Benign neck cysts and masses are usually removed by surgical excision. Head and neck cancers may be treated by some combination of radiation therapy, chemotherapy, and surgery, depending on their nature.
Reference
1. Rosenberg TL, Brown JJ, Jefferson GD; Evaluating the adult patient with a neck mass. Med Clin North Am. 2010 Sep;94(5):1017-29.
2. Pfaff JA, Moore GP. Otolaryngology. In: Marx JA, Hockberger RS, Walls RM, et al, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 7th ed. Philadelphia, Pa: Mosby Elsevier; 2009: chap 70.
3. Chen A, Otto KJ. Differential diagnosis of neck masses. In: Cummings CW, Flint PW, Haughey BH, et al, eds. Otolaryngology: Head & Neck Surgery. 5th ed. Philadelphia, Pa: Mosby Elsevier; 2010: chap 116.
| Copyright ©2017 Asia Medical Specialists Limited. All rights reserved. |
