Breast Screening: Today
Breast Screening: Today
written by Dr James Kong
(Last update on: Oct 28th 2020)
Introduction
The average woman depending on her racial ethnicity has a one in 6~9 chance of developing breast cancer during her lifetime, based on a life expectancy of 85 years. Studies have shown that regular screening of women with no symptoms has decreased the number of women who die from breast cancer by approximately 45 percent.
Traditionally, recommendations for screening have been standardised for all women irrespective of their risk groups. However today, screening guidelines for breast cancer for an individual woman should take in account those with an average risk versus those with an increased risk because of familial or genetic predisposition.
Breast screening guidelines for the ‘community’ however needs to take into account not only the relative risks but there is a need to ensure that a high quality, comprehensive assessment programme.When breast screening was introduced in the NHS in 1987 (the Forrest Report), the recommendation was that assessment should be carried out by multidisciplinary teams. Since then, guidance has been published on the organisational support that this requires and a number of standards have been included in breast screening quality assurance guidelines to ensure that this assessment is carried out satisfactorily. The present guidance sets out the minimum standards for breast screening assessment. The aim of assessment is to obtain a definitive and timely diagnosis of all potential abnormalities detected during screening.
This is best achieved by using ‘triple assessment’, comprising imaging (usually mammography and ultrasound), clinical examination and image guided needle biopsy for histological examination where indicated. Cytology should no longer be used alone to obtain a non-operative diagnosis of breast cancer [1].
Breast Cancer Risk Types
Women can be segregated into four distinct risk categories and different screening tests available to facilitate detection of breast abnormalities.
1. Average-risk women have:
- No symptoms
- No history of invasive breast cancer, ductal or lobular carcinoma in situ, or atypia, also known as atypical hyperplasia.
- No family history in a first-degree relative (parent or sibling), or no suggestion/evidence of a hereditary syndrome
- No history of mantle radiation
2. Above-average risk women have any of the following:
- Family history of breast cancer (i.e., one first-degree relative – a parent or sibling – who had breast cancer)
- Diagnosis of atypia, aka atypical hyperplasia (benign breast disease), or lobular carcinoma in situ
- History of having been treated with mantle radiation before the age of 32
Breast Cancer Screening Tests
Breast cancer screening involve a number of different types of examinations, namely:
1. Breast Self Examination
During a breast self-examination (BSE), a woman checks herself for any irregularities, which may include lumps, changes in breast size or shape, nipple discharge, or irregular tissue thickening. To date, no study has shown a statistically significant reduction. Hence BSE is no longer aggressively encouraged nor is any woman actively discouraged from performing regular BSE.
2. Clinical Breast Examination
A clinical breast examination (CBE) is an examination of the breast performed by a health professional who is fully competent in performing such an examination. In clinical studies where CBE was performed along with mammography, the reduction in deaths from breast cancer was similar to the reduction in those women who received mammography alone. This suggests that CBE adds little to mammography in reducing breast cancer deaths.
3. Mammography
Mammography is the diagnostic examination of the breast using low-dose x-rays. Annual mammogram screenings have been shown to reduce significantly the number of women dying from breast cancer in the age group 40 years and older. Until fairly recently, all mammograms used the conventional film-based technique. Today, digital mammography uses x-rays but captures the image on a computer database, where the resultant image can be viewed and manipulated for better contrast and analysis. This is becoming the standard. Although no significant difference between the two techniques when applied to the general population and for most women over 50, studies show that digital mammograms detected more cancers in three specific groups: women under 50, women with dense breasts, and women before menopause.
4. Ultrasound
Breast ultrasound is the alternative modality to evaluate breast abnormalities that are found during mammography or a clinical breast exam. The accuracy of breast ultrasound is highly operator dependent, thus creating an increased risk of false positives that requires follow-up and biopsy. This often leads to unnecessary anxiety for the patient. Again to
date, there is no data to establish that annual screening with ultrasound will reduce breast cancer mortality. For the subpopulation of high-risk women with dense breasts in whom the benefits outweigh the risks, there is an ongoing multi-center study evaluating the use of ultrasound in this group. Currently, it is not the standard of care to offer or perform ultrasound as a routine screening examination.
5. Magnetic Resonance Imaging
Magnetic resonance imaging (MRI) is an expensive diagnostic procedure that uses a magnetic field and requires the injection of intravenous contrast dyes. Recent studies of women with an inherited risk of breast cancer have shown that MRI has a higher sensitivity in detecting breast cancers than other screening methods. However, there are no study data showing that MRI will reduce the number of deaths.
Breast Cancer Screening Recommendations for Women at Average Risk
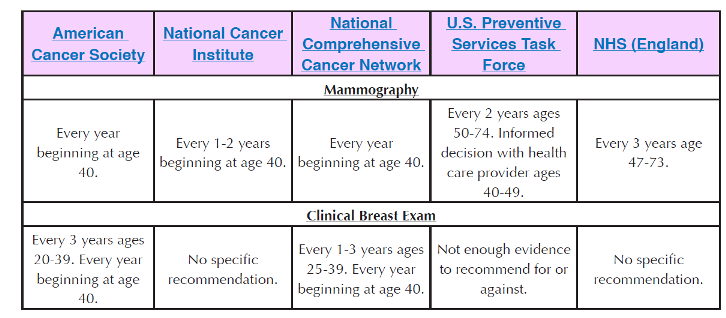
References
1. Clinical guidelines for breast cancer screening assessment. Published June 2010 (3rd Edition) | ISBN 978-1-84463-068-4
| Copyright ©2019 Asia Medical Specialists Limited. All rights reserved. |
