Gastroscopy FAQs
Gastroscopy FAQs
reviewed by YP TAI
Last update: 24th Aug 2020
What is Gastroscopy (OGD)?
Gastroscopy, also known as OGD (oesophago-gastro-duodenoscopy) is the examination of the oesophagus (In US English, esophagus, thus the procedure may be called ‘EGD’), stomach and duodenum (first portion of the small intestine) by a thin, flexible tube called a gastroscope (Fig.1), which has its own camera lens and light source. The images are viewed on a video monitor, pictures of the images can also be taken. This procedure may sometimes be also referred to as upper endoscopy, upper GI endoscopy or gastroscopy.
 Fig. 1 A gastroscope |
Why is Gastroscopy done?
It is most often used to evaluate symptoms of indigestion such as upper abdominal pain, nausea, vomiting or difficult swallowing. It can also be used to look for the cause of bleeding from the upper gastrointestinal tract. It is used for screening for stomach cancers in high-risk populations, for example Japanese.
Bariatric Intragastric Balloons (BIB) for weight-loss are placed in the stomach and inflated under OGD guidance.
OGD is more accurate than X-ray films (barium studies – Fig.2) for detecting inflammation, ulcers (Fig.3) and tumours of the oesophagus, stomach and duodenum.
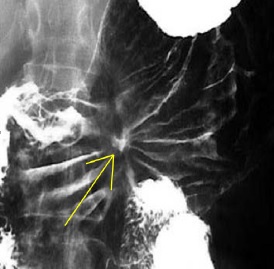 Fig. 2 Barium meal image of gastric ulcer (arrow) |
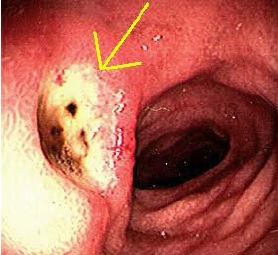 Fig.3 Duodenal ulcer seen on OGD (arrow) |
Gastroscopy (OGD) allows your doctor to obtain small tissue samples called biopsies from the lining of the upper gastrointestinal tract. A biopsy helps your doctor distinguish between benign and malignant (cancerous) tissues. Biopsies are also taken to test for Helicobacter pylori, the bacterium that causes ulcers.
Gastroscopy (OGD) can also be used to remove polyps (usually benign growths) or treat bleeding (Fig.4).
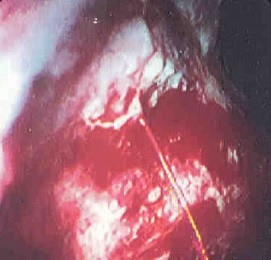 Fig.4 Bleeding gastric ulcer - blood is seen to be ejecting from the centre of the ulcer |
How should I prepare for the procedure?
Having an empty stomach is all that is required. This can be achieved by not eating or drinking, including water, for approximately six hours before the examination.
If you are taking any medications you might need to adjust your usual dose for the examination, be sure to inform your doctor. Discuss any allergies to medications as
well as medical conditions, such as heart or lung disease.
What can I expect during Gastroscopy?
The procedure is performed in an endoscopy room in a hospital or medical centre. An endoscopy nurse will spray your throat with a local anaesthetic. This is a drug that helps to numb your throat thereby minimising any discomfort caused by the endoscope. You’ll then lie on your left side, then an anaesthetist will give you an intravenous sedative to help you relax. The endoscope would then be passed through your mouth and into the oesophagus, stomach and duodenum.
Most patients go into a sleep-like state and will have no recollection of the procedure, but recover rapidly afterwards, as the drugs produce a short period of ‘retrograde amnesia’, a short period of sedation, and a quick recovery.
What happens after Gastroscopy?
You will be monitored until most of the effects of the medication have worn off. Your throat might be a little sore, and you might feel bloated because of the air introduced into your stomach during the procedure. You should be able to eat normally after the procedure unless your doctor instructs otherwise.
You should arrange for someone to accompany you home because the sedatives might affect your judgment for the rest of the day. You won’t be allowed to drive for the rest of the day even though you might not feel tired. You can return to work if you feel sufficiently alert. In general, your test results will be available on the day of the procedure; however, the results of some tests, such as tissue biopsy, might take several days.
What are the possible complications of gastroscopy?
Although complications can occur, they are rare when doctors who are specially trained and experienced in this procedure perform the test. Bleeding can occur at a biopsy site or where a polyp was removed, but it’s usually minimal and rarely requires follow-up intervention.
Other potential risks include a reaction to the sedative used, complications from heart or lung diseases, and perforation - a tear in the gastrointestinal tract lining. It’s important to recognise early signs of possible complications. If you have a fever after the test, trouble swallowing or increasing throat, chest or abdominal pain, tell your doctor immediately.
| Copyright ©2017 Asia Medical Specialists Limited. All rights reserved. |
